Effective Melasma Treatments at Shore MedSpa in Rockville, MD
Melasma is a common form of facial hyperpigmentation that produces brown to gray-brown patches, typically on the cheeks, forehead, upper lip, and chin.
This article explains what causes melasma, how clinicians classify epidermal versus dermal or mixed pigmentation, and which in-office and at-home strategies reduce visible pigment while lowering recurrence. Readers will learn how chemical peels, laser resurfacing, and adjunctive topical agents work, who is a good candidate for each approach, and what realistic timelines and maintenance look like. For local context and medical oversight, Shore MedSpa & Bio Aesthetics, led by Board-Certified Dermatologist Dr. Ronald Shore, offers tailored options including VI Peel treatments, Er:YAG laser resurfacing, and microneedling in the Rockville and Montgomery County area. The following sections define melasma, compare chemical peels and laser options, and describe why clinician-led, personalized plans matter for durable results.
What is Melasma? Causes, Types, and Symptoms Explained
Melasma is a chronic pigmentary condition caused by increased melanin production in the skin, producing irregular brown or gray-brown patches often worsened by UV exposure and hormonal shifts. The underlying mechanism involves melanocyte hyperactivity and dermal changes that can be epidermal, dermal, or mixed, which informs treatment choice and prognosis. Recognizing the type and triggers helps determine whether superficial exfoliation, topical inhibition of pigment, or deeper resurfacing is appropriate. Accurate classification also reduces the risk of post-procedure worsening and guides preventative strategies that accompany any in-office therapy.
What triggers melasma and hormonal pigmentation?
Common triggers for melasma include hormonal changes such as pregnancy and oral contraceptives, chronic sun exposure, genetic predisposition, heat and visible light, and certain systemic medications. These factors increase melanocyte activity or exacerbate existing pigment and often act together; for example, hormonal shifts combined with UV exposure commonly produce new or darker patches. Preventive measures such as strict sun protection, visible-light shielding, and reviewing medications can reduce flare frequency. Understanding reversible triggers—like stopping an offending medication or post-partum hormonal normalization—helps set realistic expectations for treatment response and long-term control.
How to identify different types of melasma and hyperpigmentation?
Clinically, epidermal melasma appears as well-defined, darker brown patches that enhance under Wood’s lamp, while dermal pigment has a bluish-gray tone and does not intensify with Wood’s lamp, indicating dermal melanophages. Mixed melasma shows both features and typically requires combination approaches for meaningful improvement. Dermatologic evaluation, including dermoscopy or Wood’s lamp inspection, informs whether superficial peels or ablative resurfacing are likely to benefit. When lesions are atypical, rapidly changing, or unresponsive to standard care, referral to a dermatologist is warranted to exclude other causes of hyperpigmentation.
Which Chemical Peel Treatments Are Effective for Melasma in Rockville, MD?
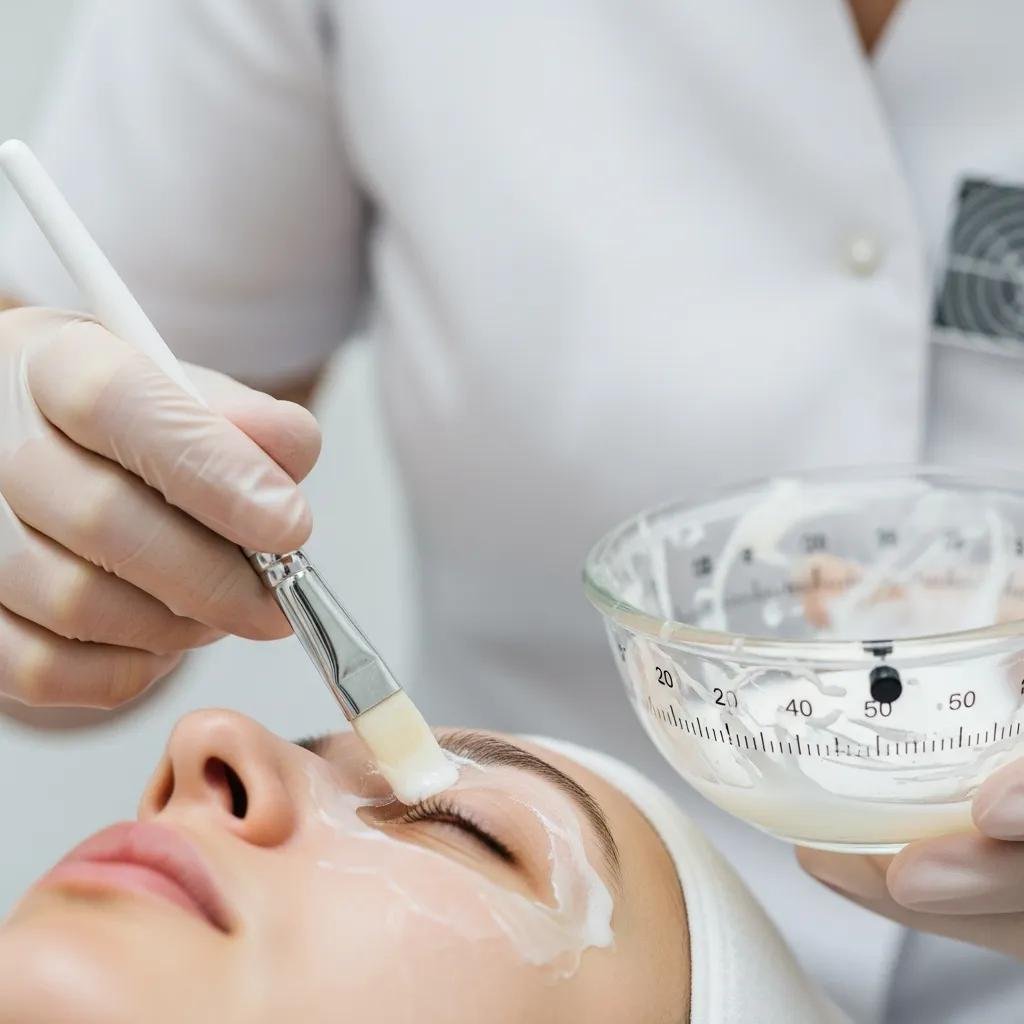
Chemical peels treat melasma by controlled exfoliation of pigmented keratinocytes and by accelerating epidermal turnover, which reduces visible pigment and improves skin texture. Superficial to medium-depth peels using alpha-hydroxy acids, trichloroacetic acid (TCA), or formulated blends like the VI Peel target epidermal pigment and can be repeated to maintain results. Suitability depends on skin type, melasma depth, and tolerance for downtime; darker Fitzpatrick types require cautious protocols to avoid post-inflammatory hyperpigmentation. Below is a concise comparison of common peel options to guide expectations and selection.
Different peel types balance depth, downtime, and suitability:
| Peel Type | Depth & Mechanism | Downtime & Suitability |
|---|---|---|
| VI Peel | Superficial–medium; combined acids and retinoid to exfoliate pigment | Minimal–moderate downtime; formulated for broad skin types with professional supervision |
| AHA (glycolic/lactic) | Superficial; increases epidermal turnover and reduces surface pigment | Minimal downtime; suitable for maintenance or mild epidermal melasma |
| TCA (low–medium) | Medium depth; stronger coagulative effect removes deeper epidermal pigment | Moderate downtime; requires careful use in darker skin tones to prevent PIH |
This comparison highlights that peels are tools to reduce epidermal pigment and improve tone, but require individualized selection and follow-through with sun protection to maintain gains.
How do VI Peels reduce melasma and improve skin tone?
VI Peel formulations combine acids and supportive agents to penetrate the epidermis and promote uniform desquamation, which removes pigmented keratinocytes and stimulates regeneration. Active components act synergistically to reduce melanin deposition and improve texture over a series of treatments, with many patients noting visible improvement within 2–4 weeks after peeling and continued gains over subsequent months. VI Peels are often chosen for their predictable depth and ability to be tailored under professional supervision, making them an option for patients seeking in-office chemical exfoliation. Because pigment can recur, VI Peel treatment is most effective when paired with ongoing topical maintenance and sun protection.
What is the chemical peel process and expected results?
A typical peel process begins with a dermatologic consultation to assess skin type, melasma depth, and risks, followed by pre-conditioning of the skin with topical agents as indicated to lower complication risk. On procedure day, the clinician cleanses and applies the peel solution, monitors response, and provides aftercare instructions emphasizing gentle cleansing, moisturization, and strict photoprotection to support healing. Expected results vary: superficial peels may need several sessions spaced weeks apart for modest improvement, while medium-depth peels produce more pronounced change but with longer recovery. Long-term control requires maintenance with topical inhibitors and sun avoidance to reduce recurrence.
How Does Laser Melasma Treatment Work at Shore MedSpa?
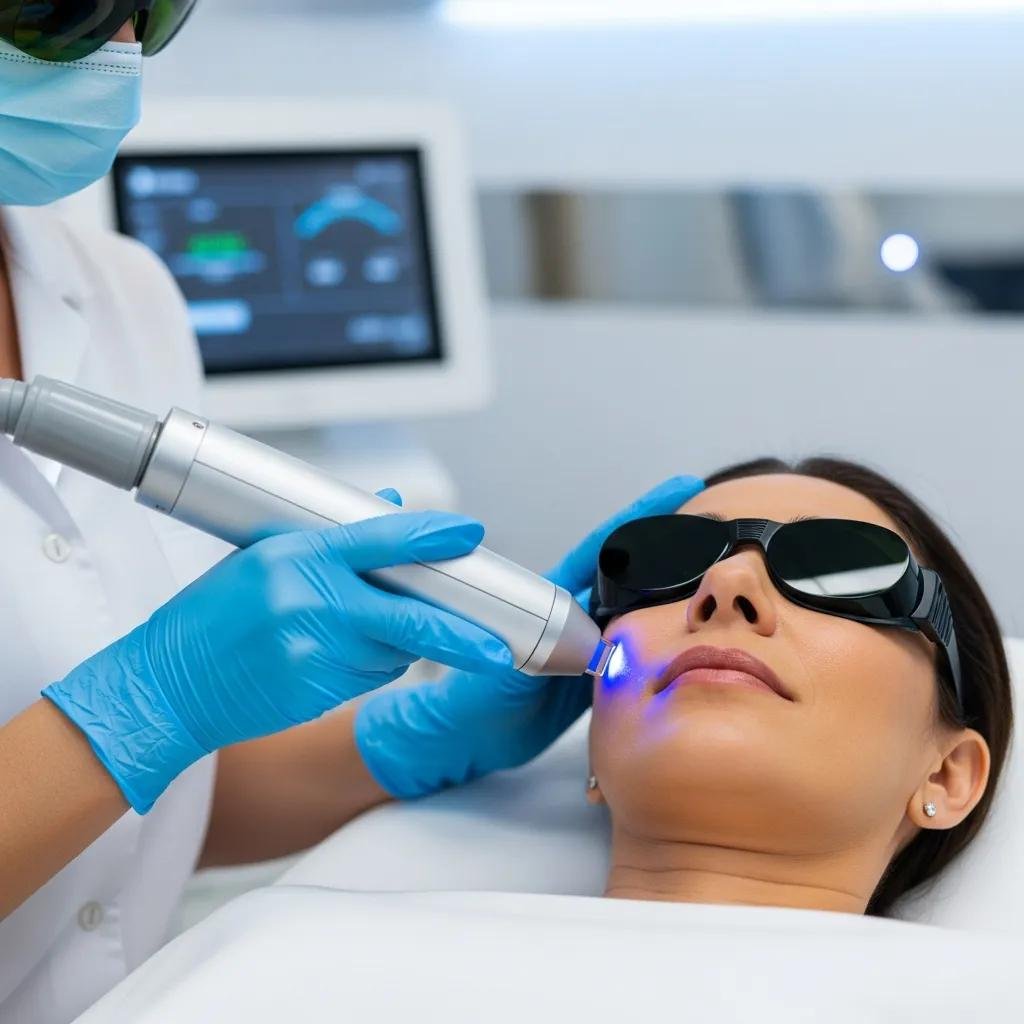
Laser therapies target pigment through selective photothermolysis or ablative resurfacing to remove pigmented cells or remodel the epidermis and superficial dermis, depending on modality. Er:YAG laser resurfacing is an ablative option that vaporizes superficial skin layers to eliminate epidermal pigment and stimulate regeneration, offering pronounced improvement for suitable epidermal or focal dermal pigment. Careful candidate selection and conservative settings are essential because inappropriate laser use can worsen melasma, especially in darker skin types. Combination approaches—pairing lasers with topical inhibitors or gentle peels—can address mixed-type melasma more effectively than single-modality treatment.
Laser modality comparison for melasma decisions:
| Modality | Mechanism | Downtime & Typical Sessions |
|---|---|---|
| Er:YAG (ablative) | Vaporizes superficial layers to remove pigment and promote regeneration | Moderate downtime; fewer sessions with pronounced resurfacing effect |
| Fractional (non-ablative/ablative) | Creates microthermal zones to induce remodeling while preserving surrounding skin | Mild–moderate downtime; multiple sessions often required |
| Q-switched/pico (pigment-specific) | High-energy pulses fragment pigment particles for clearance | Minimal downtime; variable efficacy for mixed or dermal melasma |
This table clarifies that Er:YAG is a strong resurfacing option but must be selected and performed by experienced clinicians for safe outcomes.
What is Er:YAG laser resurfacing and its benefits for melasma?
Er:YAG laser uses a wavelength highly absorbed by water to ablate superficial skin with precision, removing pigmented epidermal tissue while promoting orderly wound healing and collagen remodeling. Benefits include targeted removal of epidermal pigment, improved skin texture, and a lower thermal injury zone compared with deeper ablative lasers, which can reduce post-procedure complications when used correctly. Typical recovery involves several days to about one week of re-epithelialization, and patients often require fewer sessions than non-ablative options for comparable surface improvement. Proper pre- and post-procedure topical regimens and photoprotection are critical to sustain benefits.
Are combination laser therapies available for mixed-type melasma?
Combination strategies pair laser resurfacing or fractional energy with topical pigment inhibitors, laser-assisted drug delivery, or gentle peels to address both epidermal and dermal components of mixed melasma. These multimodal plans aim to maximize pigment reduction while minimizing recurrence by attacking different pathophysiologic steps—removal, suppression of melanin synthesis, and stabilization of the dermal environment. Clinicians weigh pros and cons such as increased complexity, cumulative downtime, and monitoring needs; careful sequencing and conservative settings reduce the risk of paradoxical darkening. For many patients with mixed melasma, a staged combination approach yields better long-term control than single therapies alone.
| Adjunct | Mechanism | Typical Use & Cautions |
|---|---|---|
| Tranexamic acid (topical/oral) | Inhibits plasmin-mediated melanogenesis | Used alongside procedures to reduce recurrence; monitor for systemic contraindications |
| Hydroquinone | Inhibits tyrosinase to lower melanin synthesis | Effective topical for epidermal melasma; limited-duration use recommended under supervision |
| Azelaic acid | Anti-inflammatory and tyrosinase inhibitor | Useful for sensitive or darker skin types; can be combined with peels or microneedling |
| Microneedling | Enhances topical penetration and stimulates remodeling | Often combined with topical agents for mixed pigment; technique must be tailored to avoid PIH |
These adjuncts illustrate how combined modalities address multiple mechanisms to improve outcomes and limit relapse when integrated into a physician-led plan.
Why Choose Shore MedSpa & Bio Aesthetics for Melasma Treatment in Rockville?
Shore MedSpa & Bio Aesthetics combines Board-Certified Dermatologist oversight with advanced procedural options—such as VI Peel formulations, Er:YAG laser resurfacing, and microneedling—delivered in a personalized care plan for clients in Rockville and the surrounding Montgomery County communities. The clinic emphasizes medical assessment to classify melasma type and skin phototype before recommending conservative or advanced interventions, reducing the risk of treatment-induced worsening. Their approach prioritizes evidence-informed modality selection, stepwise sequencing of peels or lasers with topical maintenance, and patient education on sun and visible-light protection to prolong results. Choosing clinician-led care ensures procedural safety, individualized protocols, and coordinated maintenance strategies.
- Board-certified medical oversight: Procedures are planned with dermatologic expertise.
- Advanced modalities: Availability of VI Peels, Er:YAG resurfacing, and microneedling for tailored care.
- Customized treatment plans: Selection and sequencing based on melasma type and skin characteristics.
These strengths support safer, more effective melasma management for patients seeking durable pigment reduction under medical supervision.